Covid-19 patients with high blood sugar at higher risk of death, study suggests
Covid-19 patients with high blood sugar at higher risk of death, study suggests
Mangalore Today News Network / Yahoo
New Delhi, Nov 25, 2020: Ever since the beginning of the COVID-19 pandemic, a number of underlying diseases have been associated with risks of severe disease, hospitalisation and even death.
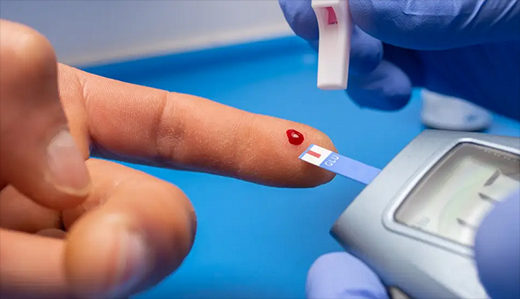
Diabetes is one of the key comorbidities associated with adverse COVID-19 outcomes, and many studies have thrown light on the various mechanisms involved in disease progression that make someone with diabetes more susceptible to severe symptoms and complications.
Diabetes, diabetic retinopathy and COVID-19
A study published in Diabetology in July 2020 revealed that COVID-19 patients with higher levels of fasting blood sugar are at risk of death within 28 days of getting infected, primarily due to older age and cerebrovascular diseases. The study data also showed that patients with fasting blood sugar levels less than 6.1 mmol/L (110 mg/dL) had a lower risk of severe outcomes due to COVID-19.
A recent study published in Diabetes Research and Clinical Practice suggests that COVID-19 patients with both diabetes and diabetic retinopathy had a five-fold increased risk of intubation. Diabetic retinopathy is a complication of diabetes in which the small blood vessels of the eye are damaged, causing mild eye symptoms and blindness when left uncontrolled. Damage to the blood vessels is anyways linked to severe COVID-19 outcomes but this was the first study to link diabetic retinopathy with intubation during hospitalisation due to COVID-19.
High blood sugar in non-diabetic patients
While the link between diabetes and severe COVID-19 outcomes is repeatedly highlighted by studies, it’s important to note that high blood sugar levels in non-diabetic patients can also lead to complications and even death. A new study published in the Annals of Medicine suggests that abnormally high blood sugar levels (hyperglycemia) at the time of admission are a strong predictor of worse outcomes and mortality in non-critical hospitalised COVID-19 patients regardless of any history of diabetes.
Previous research, including one published in the Journal of Clinical and Diagnostic Research in 2014, indicates that not all patients with hyperglycemia are diabetic and that this is a very important consideration people in medicine and surgery have to take during their regular practice. Underlying medical conditions like polycystic ovary syndrome (PCOS) and Cushing’s syndrome can cause hyperglycemia and so can stress, injury, trauma, infections like pneumonia and the use of certain medications like steroids and diuretics.
Hyperglycemia and severe COVID-19 outcomes
This type of hyperglycemia can also cause blood vessel damage and is just as likely to lead to severe complications. Add COVID-19 to the mix and the results are naturally likely to be graver if hyperglycemia is left untreated in non-diabetic patients. This is the reason why the researchers behind the new study strongly recommend that all patients hospitalised due to COVID-19 must be screened (and treated if necessary) for hyperglycemia to prevent COVID-19 complications.
To prove this connection between hyperglycemia and adverse COVID-19 outcomes, the researchers studied 11,312 patients hospitalised in centres across Spain and analysed their risk of all-cause mortality. Only 18.9 percent of these patients (2,128) had diabetes at the time of admission. Around 20.4 percent patients (2,289) died during hospitalisation, and 15.7 percent of these patients had blood glucose levels less than 140 mg/dL, 33.7 percent had readings between 140-180 mg/dL and 41.1 percent had blood glucose above 180 mg/dL. Blood glucose levels below 140 mg/dL are considered to be within the normal range.
The researchers found that the cumulative probability of mortality was significantly higher in patients with hyperglycemia - whether they had diabetes or not - as compared to those with normal blood sugar levels. Hyperglycemia was also associated with a greater requirement of mechanical ventilation and admission to the intensive care unit. The findings of this study, therefore, indicate that screening all COVID-19 patients for hyperglycemia at the time of hospital admission can help doctors provide better care and treatment to minimise all-cause mortality as well as complication risks.
- 6 Dead as massive fire engulfs Patna hotel, over 50 feared trapped, watch
- Horlicks, Boost drop ’Health’ label, rebranded as "Functional, Nutritional drink"
- Not One Vote: Mamata Banerjee’s big message after 26,000 teachers lose jobs
- On complaints against PM Modi, Rahul Gandhi, poll body’s notice to parties
- RBI plans curbs on suspect bank accounts to fight cyber fraud: Report
- Sunita Kejriwal to lead AAP’s Lok Sabha campaign in Delhi, hold roadshows
- ’Desperation born from fear of defeat’: Siddaramaiah slams Modi, defends 4% Muslim quota
- ED challenges Arvind Kejriwal’s plea in Supreme Court: ’173 phones destroyed’
- 103-year-old CSK fan flaunts love for cricket, wishes to meet MS Dhoni
- How an Indian heart saved a Pakistani teen’s life
- Zomato may soon deliver your order faster if you pay more money
- Poll body to establish over 1800 special polling booths in Karnataka
- Sullia: Rider dies in bike-jeep collision
- Mangaluru: Mustering process held ahead of LS polls
- Mangaluru: BJP accuses Congress of circulating fake pamphlet
- Over 2.88 crore voters in Karnataka to cast their franchise on April 26
- Communally sensitive DK dist was a narrative created by few: Captain Brijesh Chowta
- BJP protests against Congress government’s ‘anti-people’ policies
- Renowned Yakshagana Bhagavatha Subrahmanya Dhareshwar no more
- People must support Congress to develop DK as land of harmony: Padmaraj
- Railways to operate special trains to clear extra rush during election day
- BJP, Congress candidates end campaign by conducting roadshows in Mangaluru
- There is no Modi wave in DK: Harish Kumar
- Railways to operate election special trains from Bengaluru to Mangaluru, Kundapura
- Cops register case against ABVP activists for holding protest without permission
- New residential complex for the judges inaugurated in Mangaluru
- Absconding accused nabbed after 8 years
- Truck with cylinders turns turtle in Beltangady
- Bhoota Kola artist dies of cardiac arrest
- Development of the country should be our goal: Ganesh Karnik
- Container truck gets stuck under Modankap railway bridge
- Truck crushes bike’s pillion rider near BC Road
- Head constable dies of heart attack
- Udupi: PDO dismissed over financial irregularities
- CREDAI to resume Skill Development Program for Construction Workers in Mangaluru
- John B Monteiro elected president of Rachana Catholic Chamber of Commerce & Industry
- Sudhanshu Rai elected district president of All College Student Association
- Chief Minister to visit Mangaluru, Udupi on August 1
- Nitte University awards PhD degree to Tina Sheetal D’Souza
- Sachitha Nandagopal honoured by CMTAI for Community Service
- CITY INFORMATION
- TRAVEL
- TOURIST INFORMATION
- HEALTH CARE
- MISCELLANEOUS




 Write Comment
Write Comment E-Mail
E-Mail Facebook
Facebook Twitter
Twitter  Print
Print 

